Varicose Vein Treatment
As with most surgical conditions, treatments for varicose veins can broadly be divided into non-invasive (conservative), invasive (open surgery) or minimally invasive (endo-venous).
Conservative treatments:
These are aimed at counteracting the venous congestion due to venous incompetence. Patients with varicose veins know themselves if they can sufficiently elevate their legs the varices are far less visible and symptoms of the aching etc are temporarily relieved. This is because gravity is now no longer causing increased congestion at the capillary bed and is why people with ankle oedema notice that first thing in the morning swelling is markedly reduced.
I often explain to patients that the muscles of the calf and foot are affectively the heart of the venous system. In the same way that maintaining a healthy heart to keep the arterial system functioning well it is imperative to develop a healthy heart for the venous system. Hence the importance of exercise to maintain muscle function in the legs and feet and to maintain mobility of the knee and ankle joints.
The effect of gravity can also be counteracted by the wearing of graduated compression stockings during the day. These are constructed in a way that the compression pressure is highest at the ankle and reduces further up the calf.
Emollients to keep the dry skin moisturised can also be a helpful measure.
Whilst conservative measures can alleviate the symptoms of varicose veins they do not treat the underlying cause and are therefore not curative.
Invasive treatments:
Open surgery was a very effective treatment for primary i.e. first time treatment for varicose veins but did involve a general anaesthetic and recovery time away from normal activities and work.
Open surgery for recurrent varicose veins was technically much more challenging and carried not inconsiderable risk due to scarring around the major leg arteries and nerves.
Minimally invasive treatments:
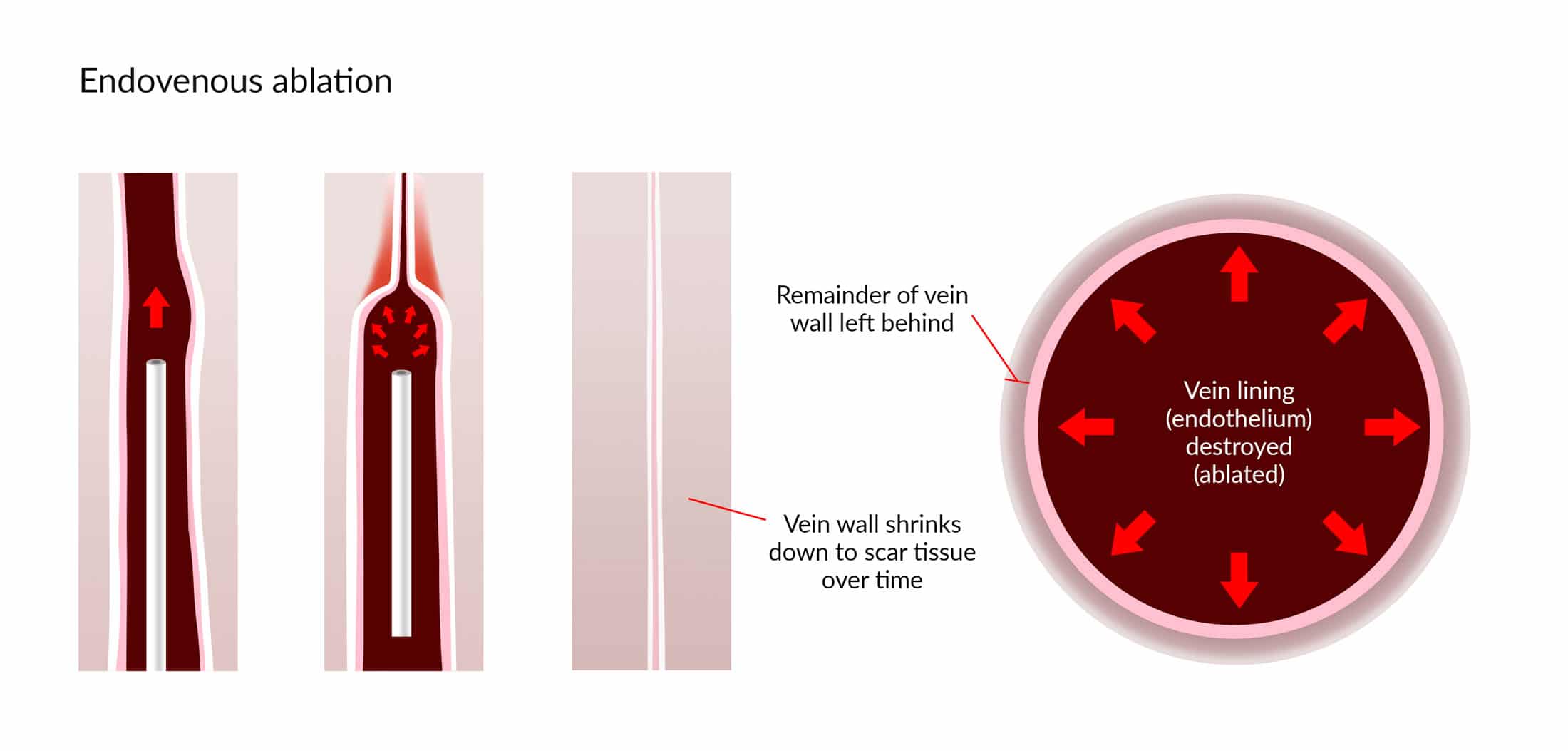
Minimally-invasive techniques are now the mainstay of varicose vein treatments. They treat the veins from the inside (‘Endo-venous’) and seek to destroy the lining of the vein (the endothelium). Without the endothelium the vein can no longer function so it ceases to transmit blood and shrinks down to become a fibrous cord of scar tissue. Various techniques involve different modalities to achieve this endothelium destruction (known as ablation).
Endo-venous techniques can be broadly divided into catheter-based and non-catheter-based.
Catheter based techniques:
These achieve destruction of the endothelium by the use of an energy source delivered via a catheter (specialised tube) passed into the vein.
The energy can be thermal i.e. the use of heat energy to effectively cook the inside of the vein, laser energy, steam, or radio-frequency energy.
Non-Catheter based techniques:
These involve injection of a chemical irritant (‘sclerosant’) directly into the vein system being treated.
Sclerosants can be used in varying strengths employing varying sizes of needles depending on the diameter of the vessel to be treated. Weak sclerosant solutions (0.2% or 0.5%) are injected in liquid form have long been known to be effective in very small veins and thread or spider veins and is the technique I use for Microsclerotherapy.
A stronger solution (1% or 3%) of sclerosant is mixed under pressure, the Tessari technique, with air or carbon dioxide (CO2) to form foam. The foam displaces blood within the larger varicose veins allowing this to be an effective treatment for varicose veins. The foam is visible on ultrasound which ensures deployment of the foam into veins requiring treatment hence ultrasound guided foam sclerotherapy (or ‘USGFS’……..we are addicted to pseudonyms in the medical field!).
At Southwest Veins we offer the minimally invasive Foam Sclerotherapy treatment.
Why choose Southwest Veins for varicose vein treatment?
We occupy an elegant suite within the Guardhouse redevelopment at Royal William Yard in Plymouth. Our clinic boasts a team of skilled Surgical Care Practitioners and is led by Jamie Barwell, a renowned consultant vascular surgeon with a track record of successfully treating hundreds of patients since 2007. If you’re from the southwest UK or further afield, our clinic offers a calming and inviting environment for your care.
What our patients say
“I consulted Southwest Veins because I had pain in the veins in one leg Jamie assured me that after treatment the pain would stop. The relief was instant and when the bandages were removed the unsightly veins had disappeared. The result was so good I had the other leg treated. I have been conscious of the veins on my legs for years now they are not a problem. I am so pleased with the results. Thank you, Southwest Veins.”
“I saw the results of a friend’s leg who saw Jamie and was amazed at the result so booked an appointment with him. For years my leg was full of bulging veins, painful and itchy, I always wore long skirts to hide them as I felt so embarrassed. From initial contact to treatment, and sending final before and after photos, Jamie was professional but friendly and done an amazing job on my awful veins. I cannot recommend Southwest Veins highly enough. I am delighted with the results.2
“Jamie Barwell has treated both of my legs for varicose veins. One leg was really pretty bad the other not quite so bad. The treatment was quick, easy, and just about painless. All the staff were very reassuring and helpful. Best of all both lots of treatment were successful. Both of my legs are now pain free with hardly any trace of any of the veins that were there. I would really recommend this treatment, by Jamie Barwell, to anyone that has varicose veins.”
FAQs…

Video appointments
Book your FREE initial consultation to discuss your varicose vein removal via video. This enables us to meet, virtually, face to face and for us to diagnose your condition and answer any specific questions.